What if your emotional and physical ups and downs had a hormonal explanation? The impact of progesterone on your body
July 11, 2025Melasma: What It Is, Why It Appears, and How to Manage It Safely
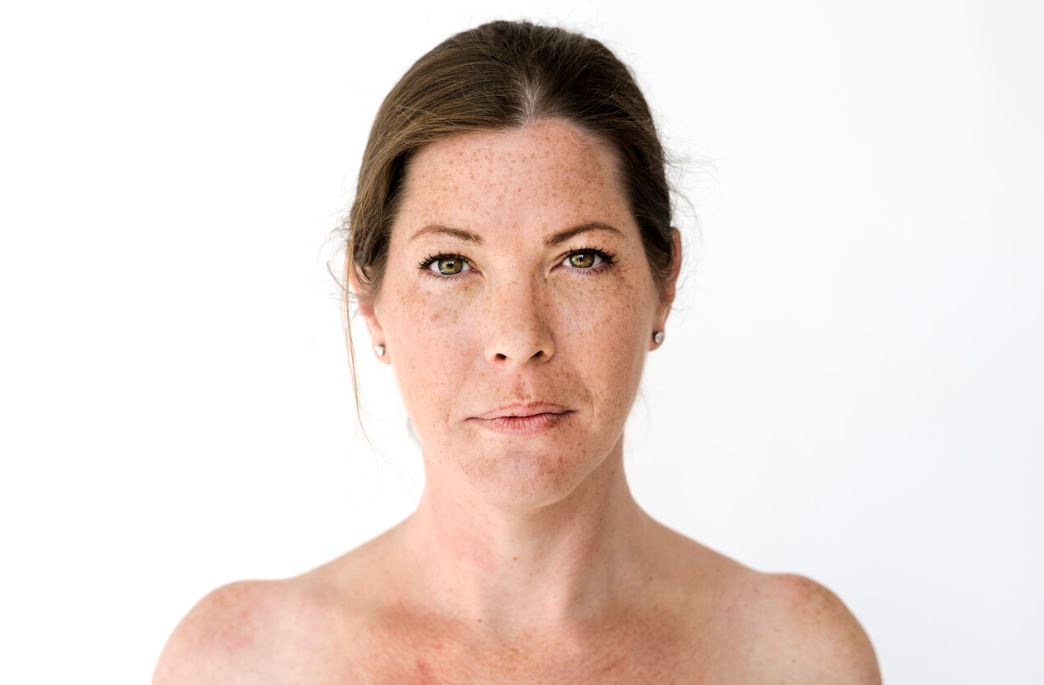
Melasma is a type of skin hyperpigmentation that shows up as brown or grayish patches, mostly on the face—especially the forehead, cheeks, upper lip, and chin. While it’s not harmful to your health, it can significantly impact your self-esteem and how you relate to your appearance.
Its onset is primarily linked to sun exposure and hormonal fluctuations. It’s more common in women, particularly during pregnancy, while using hormonal contraceptives, or throughout perimenopause. Genetic predisposition and skin type also play a role.
How can you tell if you have melasma?
Unlike other types of dark spots, melasma tends to be symmetrical, with irregular borders, and it usually appears in areas exposed to the sun. It doesn’t cause pain or inflammation, but it can worsen after summer or with continued UV exposure without adequate protection.
Can melasma be treated? Yes, but it requires consistency and professional care
There is no one-size-fits-all cure, but several effective strategies can reduce its appearance and prevent it from worsening. The most commonly used treatments include:
Daily broad-spectrum sunscreen (SPF 50 or higher): This is the most important step. Without consistent sun protection, no treatment will truly be effective.
Topical depigmenting creams: Common ingredients include hydroquinone, azelaic acid, tretinoin, or thiamidol. These help gradually fade the darker areas of skin.
Chemical peels: These procedures exfoliate the outer layers of the skin, encouraging cell renewal and improving tone and texture.
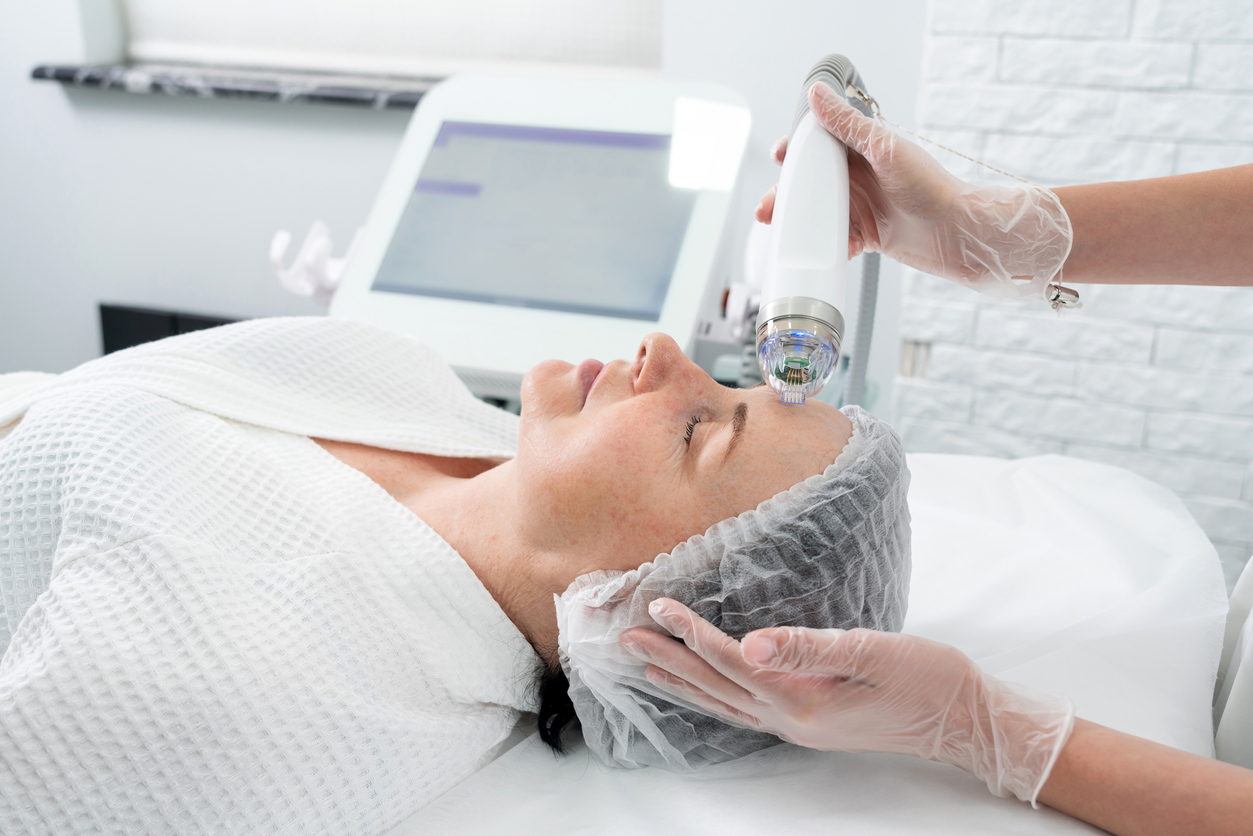
Laser therapy or intense pulsed light (IPL): Recommended for more stubborn or deeper pigmentation. These technologies target pigment in the deeper skin layers to visibly reduce discoloration.
Combination treatments: In some cases, dermatologists prescribe compounded formulas that include corticosteroids, tretinoin, and hydroquinone for a more intensive approach.
It’s essential that all treatments—especially the stronger ones—are used under medical supervision, since misuse can worsen hyperpigmentation or cause adverse effects.
Does melasma ever go away completely?
Not always. Melasma is often a chronic condition. With the right treatment and consistent care, it can improve significantly, but it can also return if those habits are discontinued.
Rather than chasing a “quick fix,” the key lies in building a steady skincare routine supported by professional guidance.
Conclusion: Your skin is not defined by dark spots—but understanding them can transform it
Living with melasma doesn’t have to be a silent struggle. Knowing that its root causes are hormonal, genetic, or environmental—and that there are medically supported ways to manage it—can change how you see your skin and how you care for it.
Your face isn’t “stained” without reason. It’s responding to internal or external factors. With the right knowledge and support, every woman can make more empowered decisions about her skin health and emotional well-being.